The Gaslighting of Science
Final Installment of the Misinformation Trifecta
Since the pandemic began, there has been a lot of talk about the supposed lack of scientific information available at the outset, a void which led to our failures to contain the virus. The science has evolved, this line of thinking goes, allowing us to pursue the proper mitigation strategies.
On the one hand, of course, that is true for any event like this. Especially one so dramatic, involving a global pandemic with a novel pathogen. We learn more as events proceed.
On the other hand, that’s not a completely accurate reflection of what happened. A lot of what was known from very early on took months, if not more, to make its way into our public health guidelines. Some are still being debated, to great frustration.
Perhaps one the most striking examples of all this is what happened with what we learned, and refused to learn, from the Diamond Princess cruise ship in February of 2020, a tragic natural experiment if there ever was one. Thousands of people were trapped inside a cruise ship as the disease spread. Besides the tragedy, it allowed us to observe what happened with the coronavirus inside a closed environment, revealing many things that could be harder to discern in a large, open city.
I recently watched the HBO documentary on the cursed cruise ship, which was one of the first big outbreaks with global attention. It was, of course, a tragedy: what started with single reported infection ended with 712 known infections and 14 deaths. When it was ongoing, in early February, it was the biggest outbreak outside of China, accounting for half the known cases.
It all started on February 1st, when the first passenger who had disembarked six days earlier was confirmed to have been infected. By February 10, at least 135 people were confirmed to have been infected in a rapidly growing outbreak despite all the passengers being entirely quarantined in their rooms. Despite the quarantine, 567 of the total 2,666 passengers on the ship eventually tested positive.
The first crucial piece of information needed to contain this disease has been the fact that it transmits from people without symptoms. In the HBO documentary, the ship’s doctor reiterates that by February 9th, he was sure that people without symptoms were infecting others. That fact had already been reported in scientific papers, urgently proclaimed by China’s minister of Health in January of 2020, apparent from multiple epidemiological reports already in the record. But many experts in the Western world found that difficult to believe (a topic I covered before for this newsletter), and we did not act upon this crucial piece of information until much later in the pandemic (I wrote about transmission from people who were not sick, and thus could not know they were infected, in March of 2020 in my first op-ed calling for masks—it was so clear even then that I had no problem convincing the fact-checkers at the New York Times).
Watching the documentary, it also becomes very clear that the disease is airborne. There really is no other reasonable explanation for how 567 passengers confined to their rooms, served food by heavily masked people, would get infected at that scale that quickly. In fact, this airborne transmission was quickly discerned by scientists around the world. One of the architects of Japan’s mitigation strategies, Dr. Oshitani, had told me that this was the case that convinced him that the pathogen was airborne (I had interviewed him for this article on aerosol transmission and ventilation for an article I wrote last July).
But it wasn’t evident just to a select few. Here’s an interview with a BuzzFeed science journalist explaining it in a pretty straightforward way on February 23, 2020:
GARCIA-NAVARRO: Cruise ships, as you wrote, are notorious for spreading illnesses. I have to start by asking, are epidemiologists really surprised that after two weeks, more than 600 people have been infected on one ship alone?
VERGANO: The people we spoke to who've studied this sort of thing in the past aren't surprised at all. And it sort of keyed on the question of, how does this virus behave? And now it's becoming apparent - or it seems apparent - we have to be very careful...
GARCIA-NAVARRO: Right.
VERGANO: ...That it's more like the flu, like influenza A, where airborne transmission earlier in an infection - during the sneezing rather than coughing stage - seems to be a factor here. And that brings into play the question of how this ship was ventilated and, you know, airborne transmission in general.
GARCIA-NAVARRO: Well, let's talk about the ventilation system.
VERGANO: So the people who've studied this - and one of the surprises here was that there actually has been a lot of research looking into this question - say that ventilation systems on cruise ships aren't any good at stopping airborne diseases from spreading, that there've been studies of flu where you have, in a week's time, you know, one patient infecting 40 people. And likewise, the air filters simply aren't designed to screen viruses. After a while, the whole system gets gunked up with it. And just speaking, sneezing, coughing in your ward room - that gets picked up by the air system, you know, and...
GARCIA-NAVARRO: And it doesn't get filtered out and maybe gets passed on.
VERGANO: In the past, that's what's happened. And unless this cruise ship had some kind of impossible-to-have ventilation system, that was going on.
For reference, here’s the contact tracing data on the ship from Japan from February of 2020 which clearl yshows that non-close contacts are playing a significant role:
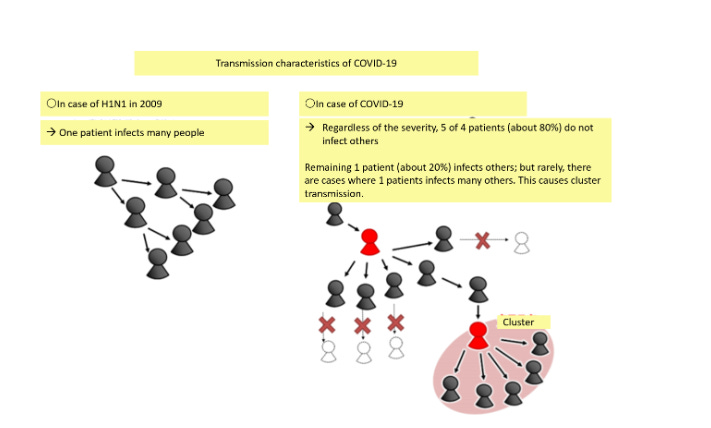
The third crucial piece of the puzzle of transmission was determining whether this pathogen behaves like flu (like the H1N1 in 2009), which spreads in a fairly uniform way, or if it was overdispersed, meaning that a few people infect many in clusters. (Here’s an article on that topic I wrote later in 2020).
The overdispersion was harder to discern from Diamond Princess alone. But on that puzzle, too, the early contact-tracing from multiple countries was already clear, that clusters were playing a big role. So clear that here’s the graphic on the role of clusters Japan was already including, in February of 2020, in its documents for contact-tracers:
And here’s a paper that was published officially by June 30th, but had been available since February of 2020 describing the approach:
Put all three together: airborne transmission, clusters driving the epidemic, and presymptomatic transmission. Not only do we get a clear and consistent picture of many things that have happened since, we also get the mitigation strategy. Further, all three dimensions support each other: transmission from people not (yet) coughing or sneezing very much argues in favor of aerosol transmission, which explains how large clusters can be driving the epidemic and how transmission in a situation like that ship can occur. And the mitigation and other strategies become clear: pay attention to clusters and ventilation, universal masks, different policies for indoors and outdoors, etc.
But all that happened far away, you might be thinking. We didn’t have examples like that to study here, and there might have been language differences and other barriers. That’s not even really true, as a lot of these papers got published in English as well, but let’s put that aside for a moment. Take a look at the Skagit Valley Choir case in Washington state. Careful, pandemic-aware people showed up at a huge space—distanced, no hugs, hand-sanitizers everywhere—and 53 of them got infected in one evening. They had even propped the door open to avoid knob touching. And yet, this event was not seen as definite evidence of aerosol transmission. It was not even seen as a definite evidence of rare aerosol transmission—a position that would still be wrong, but at least plausible, essentially arguing that happened but it was a one-time thing.
I am not linking to all those who argued against the facts, because focusing on individuals is not correct. But multiple experts insisted for a long time that the infections might have resulted from close contact or fomite transmission during break, or been the result of snack sharing. The CDC report on the Skagit case mentions aerosols as a possibility, but just that: a possibility and emphasizes how fomites and contact were possible as well.
However, as a recent Times article on choir case notes, aerosol scientists had immediately noticed what had happened, and what was actually likely, and what was really a stretch:
If, as the C.D.C. and the World Health Organization were then insisting, the virus was passed mostly through contaminated surfaces, known as fomites, or droplets exhaled from an infected person that would fall within six feet, how and why did so many members of the Skagit Valley Chorale get sick? Could all 53 of them really have touched the same door handle, or orange, or folding chair? Had all of them stood face to face, talking to one another, less than two yards apart? Intuitively, the choristers knew what must have happened: The virus had drifted throughout the room and lingered in the air they breathed.
Eager to make sure others could learn from their experience, Burdick and the chorale leadership readily agreed to interviews. On March 29, an article appeared in The Los Angeles Times that described their rehearsal. One of the millions of readers who saw the story was Jose-Luis Jimenez, an aerosol scientist at the University of Colorado, Boulder. He and nearly 40 of his colleagues were trying to get the W.H.O. to acknowledge that the virus was being transmitted through aerosols — particles that can stay aloft and float considerable distances. (U.S. officials had been playing down this prospect. In late February, the C.D.C. director, Robert Redfield, said the widespread wearing of masks was unnecessary; in early March, the National Institute of Allergy and Infectious Diseases director, Anthony Fauci, said much the same.) Jimenez dashed off a note to the reporter, Richard Read, and described the case as “the clearest example of that potential mode of transmission.” He wanted to investigate. Read connected him with Carolynn Comstock, who provided answers to a long list of questions about where everyone sat and what they touched.
Dr. Jimenez did indeed do the necessary investigation and publish a very good paper, tracing what had happened. I’ve since interviewed, and later collaborated with Dr. Jimenez (on an upcoming paper in The Lancet—it will be out soon) and he’s certainly outspoken (as he should be!) but my experience is that he’s been very open to debate and consideration of all evidence. Here’s how he describes it to the New York Times:
The outbreak also provided crucial evidence for scientists seeking to understand how the virus was being transmitted. In the months that followed, Hamner and Jimenez, along with their respective colleagues, published separate studies of the Skagit Valley case. Hamner’s, which appeared in the C.D.C.’s Morbidity and Mortality Weekly Report last May, noted that “the 2.5-hour singing practice provided several opportunities for droplet and fomite transmission, including members sitting close to one another, sharing snacks and stacking chairs at the end of the practice.” But the notion that those activities caused so many infections, as Jimenez characterized it to me, is “absurd.” He says that that emphasis helped enable the W.H.O. and the C.D.C. to maintain and defend their guidelines. They have since revised them to acknowledge that the virus is transmitted by aerosols — the W.H.O. on July 9, the C.D.C. on Oct. 5. But many scientists, Jimenez included, argue that they still haven’t stressed enough that inhaling aerosols is the dominant mode of infection, which has led entities like schools and public-transportation agencies to put time and money into cleaning regimens that would be better spent on masks and ventilation. “We proved how you get this thing,” Comstock told me. “And it’s so damn frustrating to watch the news and see that they’re ignoring it.”
As I said on Twitter upon reading this article, to imagine fomites playing a major role in such a case—transmission to 90% of the careful, distanced people present in a large space in a single evening—requires contortionist thinking, to put it politely.
And although this may seem hard to believe, contortionist thinking is exactly what we encountered for a long time. Alternative explanations were tossed out: What if the people shared snacks? What if it was the folding chairs? What if, what if, what if? Unlikely, if not downright impossible scenarios kept being raised as reasons for doubt, rather than accepting the evidence that had been screaming at us, not just from one case either but from multiple streams of evidence, all over the world.
Dr. Jimenez had a recent thread on his experiences. Something he said in the thread really struck me:
It’s not a good moment when a prominent scientist—who was, along with others, evidence-based, correct and prescient on a topic of great importance within his expertise—feels the need to look up “gaslighting” because he is lacking the word to otherwise describe his experience.
I realize that there is a lot of focus on misinformation that we recognize: the claims of 5G spreading via vaccines, of many deaths following vaccination, claims that vaccines don’t work at all, or even the idea that vaccines might have caused the death of a 99-year old, already visibly infirm, prominent member of the royal family in the United Kingdom. I understand all that and the role of such misinformation. But as I close the misinformation trifecta series about problems beyond the ones that are “over there,” committed by others, I’d like us not to forget what actually happened in more mainstream and arguably more important circles, and is still influencing how we have been responding—and failing to respond—to this pandemic.







Terrific. Particularly like this: "I am not linking to all those who argued against the facts, because focusing on individuals is not correct."
But I also have a question. What motivated the reasoning of those who opposed the pretty clear thesis of aerosol borne transmission? Why?
And, though I generally agree with the idea of not naming namse. I will name two: President Trump, who said to Bob Woodward in early February 2020: “It goes through air, Bob. That’s always tougher than the touch." It has to be said that Woodward held that information to himself for 7 months!! (before his book publication).
I recall walking through the New Orleans airport in early March 2020, wearing an N95 mask and getting all kinds of strange looks. At the same time Mike Pence and Dr. Fauci were on CNN defiantly proclaiming that masks “were not necessary for average Americans.”
A giant problem in our discourse is that the media often engages us in a lively debate, but only within certain parameters. In this case it was Trump vs. Fauci, and everybody took a side. Since neither provided a comprehensive analysis of aerosol spread, it didn’t resonate with the public or even many public health experts.